Key to ‘superbug’ antibiotic resistance discovered

Dr Matthew Belousoff and Professor Trevor Lithgow
An international study led by Monash University has discovered the molecular mechanism by which the potentially deadly superbug ‘Golden Staph’ evades antibiotic treatment, providing the first important clues on how to counter superbug antibiotic resistance.
‘Superbugs’ are bacteria that are resistant to commonly used antibiotics, presenting a global health threat. To tackle this global challenge, researchers from Monash’s Biomedicine Discovery Institute (BDI) are collaborating with Israel’s Weizmann Institute of Science, and the NTU Institute of Structural Biology in Singapore.
Now, the Monash BDI researchers have identified the first important clues on how to 'retool' antibiotics to counter the strategies bacteria enlist to evade the life-saving drugs, with the findings published in the journal mBio.
Researchers used the latest generation electron microscopes at the Monash Ramaciotti Centre for Cryo-Electron Microscopy to image at the molecular level – for the first time – the changes that take place in superbugs that have become resistant to the most modern antibiotics.
Examining bacterial samples of antibiotic-resistant Staphylococcus aureus or ‘Golden Staph’ taken from a hospital patient, they compared data of a non-resistant strain with their counterparts overseas. These included Shashi Bhushan from NTU, and Zohar Eyaland Nobel Laureate, Professor Ada Yonath from the Weizmann Institute who won the Nobel Prize for Chemistry in 2009.
“Using the combined data we could rationalise how the bacteria escapes drug treatment by a really important hospital antibiotic and describe in molecular detail how it becomes like a superbug,” said Monash BDI scientist and lead researcher Dr Matthew Belousoff.
“The bacteria mutates or evolves to change the shape of the molecule to which the antibiotic would bind so the drug can no longer fit there,” Dr Belousoff said.
“Knowing what your enemy is doing is the first step to the next phase of new drug design,” he said.
“We’ve developed a technique that others can use that might help us speed up the arms race of antibiotic development.”
Dr Belousoff said Monash BDI researchers are now using this new tool to investigate other drug-resistant bacteria.
The research, involving the expertise of Monash microscopist Dr Mazdak Radjainia and mentoring of Professor Trevor Lithgow, was supported by the Australian National Health and Medical Research Council (NHMRC).
Read the full paper titled Structural basis for linezolid binding site rearrangement in the Staphylococcus aureus ribosome
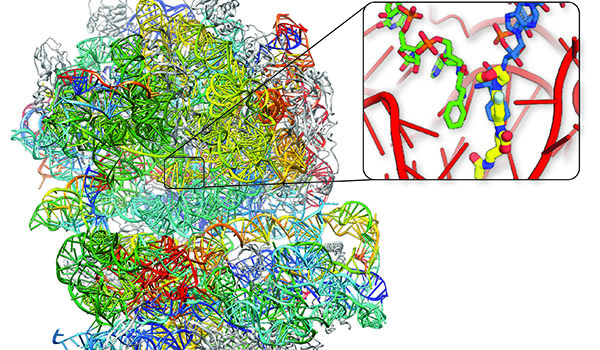
Caption - The protein-making machine from Golden Staph, the bacterial ribosome (Main picture). It is this nano-machine that evolves to escape treatment by antibiotics, which are small chemicals that have the ability to turn this machine off, by literally throwing a spanner in the works (inlay picture)
Background information
The World Health Organisation has warned that new antibiotics were urgently needed to counter the growing threat of superbugs. It predicted that deaths from antimicrobial resistance could rise to 10 million by 2050, surpassing the total deaths caused by cancer and diabetes combined. If antibiotics lose their effectiveness, surgery and even treatment of wounds could become life-threatening.